Table of Contents (click to expand)
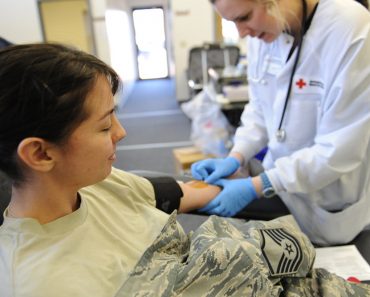
Blood transfusions take a relatively long amount of time due to precautions against negative allergic reactions, damage to the blood products, or specific medical conditions that may require a slower pace.
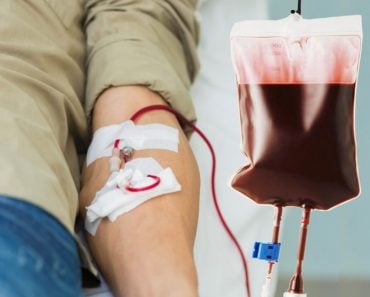
If you have ever needed a blood transfusion, after surgery or an accident, or because of a particular medical condition, you know that it can be a boring process. Once the nurse hooks your arm up to the bag of blood, the process can take up to 4 hours, or even longer! Given the fast pace of the modern world, and the rapidity of so many other medical procedures, many people wonder why blood transfusions still take so long!
Well, considering the delicate nature of this common procedure, and its potentially life-saving impact, you will better appreciate the time it takes to carry out once you learn a bit more in the course of this article.
Recommended Video for you:
What Is A Blood Transfusion?
A blood transfusion is a means of adding blood to the body, typically in the case of illness or injury, when the body is lacking or unable to maintain healthy levels of blood. An average person weighing 150-180 pounds will have an average of 1.2-1.5 gallons of blood at any given time. The body is able to rapidly produce more blood—millions of new blood cells per minute!—but in the case of a high volume of blood loss (i.e., more than 2-3 pints of blood), a transfusion will typically be required.
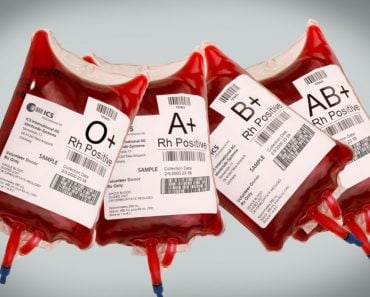
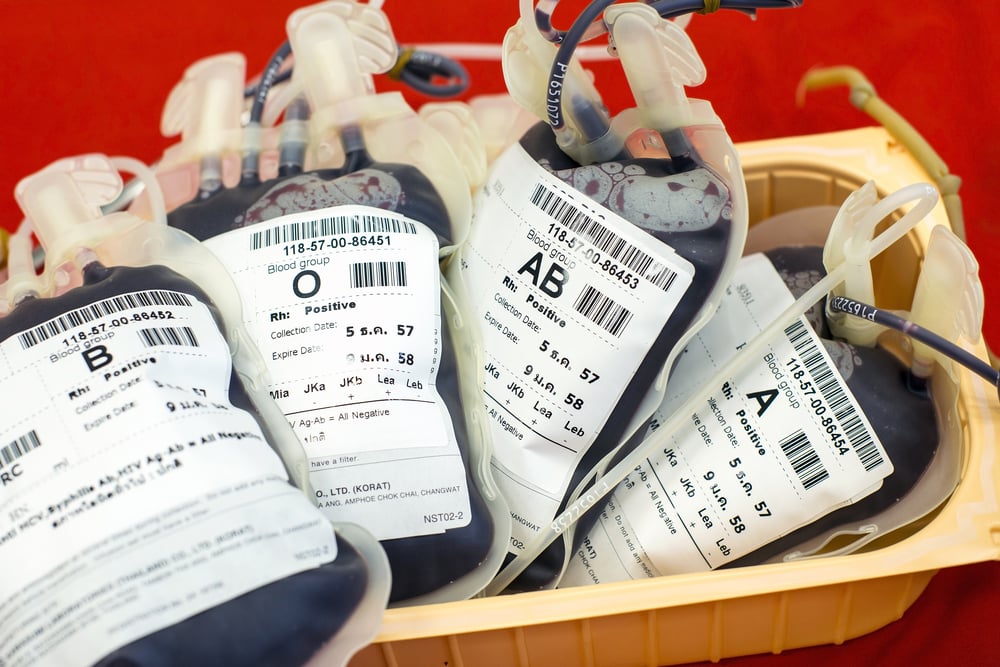
An important consideration in any blood transfusion is that the blood being given is the same as the blood type of the individual. The common blood types are A, B, AB and O, along with an Rh factor (+ or -) designation.
One must ensure that these characteristics match, or else the body will reject the donated blood, attacking it with antibodies that do not recognize the antigens on the blood cells themselves. Blood that is donated to blood banks is carefully screened, checked and categorized to prevent mismatched transfusions and potential blood-borne infections.
Not All Blood Transfusions Are The Same
Not all blood transfusions are the same, because there are four different blood products to consider. “Whole blood” is what most people donate at blood banks and blood drives, but this is only one of the possible donation types.
Our “whole blood” is composed of red blood cells, white blood cells, platelets and plasma, but many different patients will require only one of those products, not all of them. For example, if a patient’s white blood cell count is dangerously low, in the case of chemotherapy patients, they can receive a transfusion of white blood cells, rather than additional red blood cells or platelets that they aren’t lacking. Having a reliable supply of whole blood and individual blood products is important to provide emergency care in a timely manner.
While traumatic injuries or surgeries often demand the use of blood transfusions, there are also a number of medical conditions that may require the one-time or regular transfusing of your blood. Some of these illnesses include anemia, sickle cell disease, cancer, liver disease or a wide variety of blood disorders. The varied types of blood transfusions and their purpose can affect the speed at which the transfusion is allowed to proceed, as explained below.
Why Do Transfusions Take So Long?
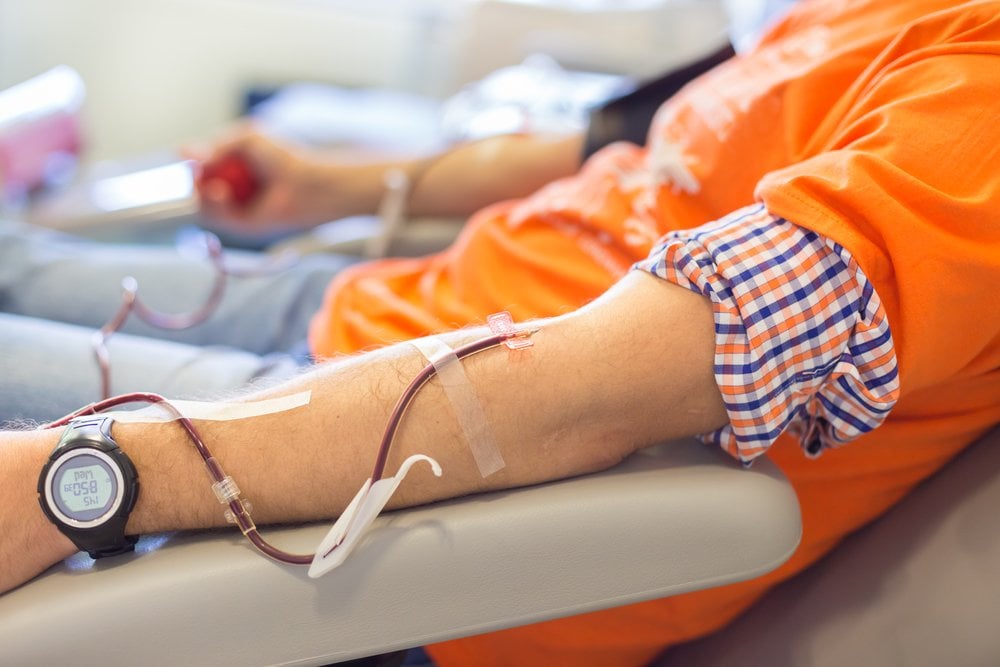
Most blood transfusions take between 1-4 hours, depending on the type of blood product, but this speed can vary in different cases, such as during an emergency or once a patient has shown they are not experiencing any negative side effects. If you are in need of large volumes of whole blood, the transfusion may take longer. Increasing the rate of transfusion can potentially damage the blood cells as they enter the body. However, if you are only getting a transfusion of platelets or plasma, the process can be carried out much faster.
In the case of an emergency, particularly if the patient’s life is in danger or the bleeding is continuous, blood can be more rapidly transfused. In such a case, the potential side effects of rapid transfusion are outweighed by the need to save the patient’s life.

Generally, however, the process is slow because a patient must be monitored at the beginning of a transfusions, for at least the first fifteen minutes. In most cases, if a negative reaction is going to occur, it will be in that initial window, at which point the nurse can cease the transfusion and identify the issue. While blood is carefully checked and correctly matched with patients’ blood types, there may still be mild allergic reactions or sensitivities in some recipients.
There are some more rare and severe side effects, such as chills, dizziness, itching, nausea, tightness of the throat, fever, respiratory and heart issues, or a situation in which the donor blood’s white blood cells begin to attack the body’s blood cells. Additionally, if patients have circulatory issues that make it difficult for them to regulate their blood fluid levels, the slower introduction of new blood is required.
Unexpected side effects during blood transfusions are rare, but when negative reactions are detected, they must be dealt with quickly. Keeping the initial flow of blood low, in case one of these side effects arises, partially contributes to the seemingly sluggish process of blood transfusion. After this initial window, if the patient’s vitals appear stable and unchanged, a nurse may increase the transfusion speed at her own discretion.
However, as mentioned at the top of the article, an average of 1-4 hours is required for transfusions in non-emergency settings, to ensure the safe delivery of undamaged blood, depending on the type of blood product and medical need.
A Final Word
The experience of getting a blood transfusion is rarely pleasant, as it typically indicates a traumatic injury, surgery, or chronic illness, but it wouldn’t be wise to speed up the process. In order to ensure that your body is reacting well to the donor blood, to avoid exacerbating existing health conditions, and to protect the integrity of the blood itself, patience is an essential virtue when it comes to blood transfusions!
References (click to expand)
- Blood transfusion - Mayo Clinic - kcms-prod-mcorg.mayo.edu
- Blood Transfusions in Adults - Health Encyclopedia - URMC. The University of Rochester Medical Center
- Treatments for Blood Disorders | NHLBI, NIH. The National Heart, Lung, and Blood Institute
- Maxwell, M. J., & Wilson, M. J. A. (2006, December). Complications of blood transfusion. Continuing Education in Anaesthesia Critical Care & Pain. Elsevier BV.