Table of Contents (click to expand)
Too tired to read? Listen on Spotify:
Even though a difference in blood groups does not affect the couple, it could become a problem while trying to conceive a child.
There are many things to keep in mind when choosing your life partner. One such thing is the blood group. We don’t think of this at first, but differences in blood groups can lead to complications. More specifically, these problems can occur during pregnancy and put the unborn child at risk.
Recommended Video for you:
Blood Group Systems
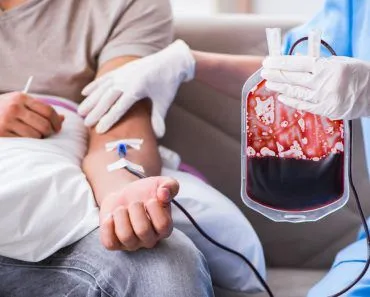
To donate blood, the nurses need to know your blood type. You may say, “I am A+,” or “I am B-.” But what do these letters and signs indicate? These two things are simply indicators of your blood groups, specifically the ABO system and the Rh system. Apart from that, we have about 30 other blood group systems.
ABO Blood Group System
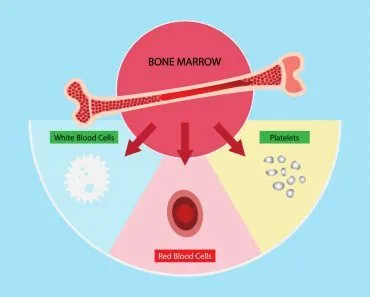
The ABO system is based on the presence or absence of antigen A or B on the surface of your red blood cells. An antigen is a molecule that triggers an immune response. Immune cells will create antibodies against the antigen.
If you have the A blood group, your red blood cells have the antigen A and vice versa for the B blood group. But what if your blood group is AB or O? The AB blood group indicates that you have both antigens A and B, whereas the O blood group indicates that you have neither of them.
If your blood group is A, your body will identify B blood group cells as foreign particles and form antibodies (anti-B) against B cells. In the same way, those with B blood will produce antibodies (anti-A) against A blood group cells. These antibodies (anti-A and anti-B) trigger an immune reaction when they encounter their respective antigens. The immune reaction can be severe and even lead to death.
Those with AB blood group do not produce antibodies against either antigen since their body recognizes both the antigens are self. This means that any other blood group can transfuse blood to AB blood group individual with little consequence and are called universal acceptors.
On the other hand, O blood group individuals will produce antibodies against both A and B antigens. But, since those with O blood group have neither A nor B antigens, they can donate blood to people with other blood groups and are called universal donors.
Rh Blood Group System
The Rh system has over 50 antigens. There are 5 that are common in humans: D, C, c, E, and e. Of these, D is the most important antigen in the Rh system. The presence or absence of the D antigen is indicated by a plus or minus sign. If a person with Rh-negative blood is exposed to Rh-positive blood, the body produces antibodies against the Rh-positive cells. However, if Rh-negative blood is transfused into an Rh-positive person, no reaction occurs as there are neither antigens nor antibodies.
Thus, if you say that you are ‘AB+’, you have the antigens of A, B, and D, but if you say you are ‘O-,’ it indicates that you have none of the antigens and all of the antibodies.
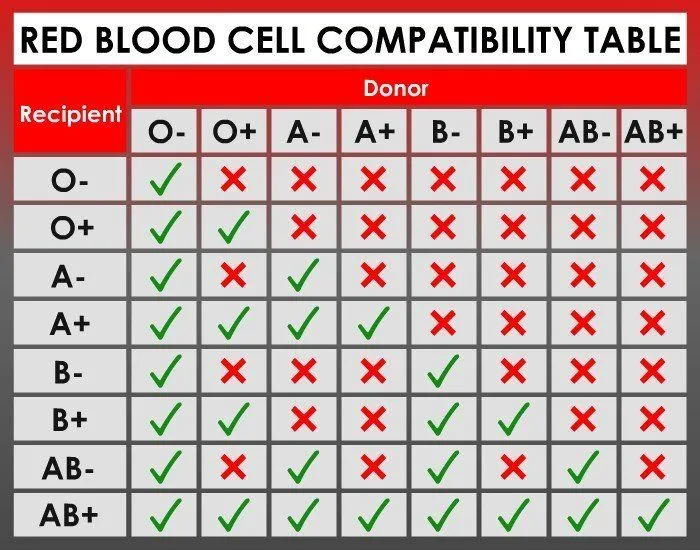
Why Is It Important To Compare Blood Groups With Your Spouse?
Even though a difference in blood groups does not affect the couple, it could become a problem while conceiving a child. The differences in the ABO system are not a major concern, but the same cannot be said for the Rh system. Rh incompatibility is a real problem, one that can affect both mother and child.

Different Blood Groups Cause Rh Incompatibility.
Rh incompatibility can occur when the mother is Rh-negative, and the fetus is Rh-positive. If the fetal blood (which is Rh-positive) leaks into the maternal circulation (which has Rh-negative blood), fetal cells will be recognized as foreign. This results in the mother producing antibodies called Rh immunoglobulin G. These antibodies could pass through the mother’s placenta and attack the fetus’s red blood cells. Once the red blood cells break down, they produce bilirubin, which causes the child to be jaundiced.
In most of these cases, the leakage of fetal blood into maternal circulation takes place during delivery. Because of this, the mother does not produce enough antibodies, leaving the first-born baby unharmed. The severity of such a situation will continue to increase with every consecutive pregnancy involving an Rh-positive fetus. The worst-case scenario would lead to marked anemia or stillbirth.
How To Treat Rh Incompatibility?
If the affected baby is born, then hydration and phototherapy using bilirubin lights can treat jaundice. Bilirubin lights (emitting rays of 420-470 nm) convert bilirubin into a form easily excreted from the body.

In the worst-case scenario, the baby might have to undergo a blood transfusion while still in the uterus. A needle is inserted into the umbilical cord, which is controlled using an ultrasound machine. The transfusion procedure takes place once in two to three weeks before the child is born.
Even if the treatment options are good and give positive results, prevention is still a better option. Rho(D) immune globulin is a medication used to prevent isoimmunization in mothers. If there is an indication that there is a chance of Rh-positive cells entering maternal circulation, it is administered at 28 to 32 weeks into the pregnancy and again within 72 hours of delivery.
Prevention of Rh incompatibility is much easier than the difficulties faced during the treatment. Couples need to check themselves for possible incompatibilities so that they know in advance what steps to take. Furthermore, advances in the commercial production of antibodies have helped reduce drug costs and increase their availability. Such steps have also reduced the probability of Rh incompatibility from 10-20% to 1%! This has opened up many possibilities for couples who want to avoid such complications.
References (click to expand)
- Rh Blood Group System - faculty.madisoncollege.edu
- ABO BLOOD GROUP SYSTEM - faculty.madisoncollege.edu:80
- N Antonios. Rh Incompatibility in Pregnancy. Arizona State University
- Blood Tests | NHLBI, NIH. The National Heart, Lung, and Blood Institute
- Rho(d) immune globulin (Injection) | University of Maryland Medical Center - umm.edu