Table of Contents (click to expand)
One symptom of rabies is a fear of water. This fear is caused by the patient’s inability to swallow liquids, as the muscles controlling that action undergo spasms that are painful due to the rabies virus.
Mouth open, saliva dripping, teeth bared, muscles tensed, and eyes red, a rabid dog terrorizes a sleepy town. The children are ushered inside their homes. Its madness is driving it to bite and tear into anyone who comes near it.
The cause for this behavior is the rabies virus. This small 5-gene, 12 kbp RNA virus causes “insanity” in its victims, all to enter another host. Humans infected with the rabies virus also show a human version of the rabid dog’s behavior: aggressive, hyper, and hydrophobic.
Popular media gets much wrong about diseases, but the fear of water or hydrophobia that rabies patients suffer from is a true symptom of the disease. It is a unique and perplexing symptom. What’s behind this behavior? How can such a microscope, not-even-alive organism, change a human’s behavior?
Recommended Video for you:
A History Of Rabies
Ancient cultures were well aware of rabies. The Greeks knew it as Lyssa (rage) or hydrophobia (fear of water). The Romans gave us the name rabies, after the Latin word rabere, meaning rage. The frenzied rage has always stood out to us.

There was no cure or treatment for rabies until Louis Pasteur came onto the scene. Over a series of experiments, Pasteur managed to weaken the virulence of the virus until it was safe enough to function as a vaccine. On July 6th, 1885, Joseph Meister, a 9-year-old boy bitten by a rabid dog, was brought to Pasteur. Since then, getting vaccines for rabies has saved countless lives.
How Does The Rabies Virus Cause Disease?
Rabies symptoms appear after a window of a few weeks. This is the incubation period. After this, flu-like symptoms appear. During this time, the virus has entered the body and will soon infect the neurons, the cells that make up the nervous system. The virus uses the neurons to travel to the spinal cord and the brain.
Once the virus reaches the brain, it begins to multiply.
Viruses multiply by hijacking the cellular machinery of the host cells to make more virus copies. Every cell has proteins, the so-called machinery, to make more DNA and proteins. The virus uses that machinery to make more copies of itself till, eventually, tens of thousands of new viruses break out of the cell, killing it in the process.
The rabies virus, replicating in the brain, infects neurons. The patient develops encephalitis, which is when the brain is inflamed. The later-stage symptoms that we associate with rabies—aggression, hyperactivity, and hydrophobia, appear now.
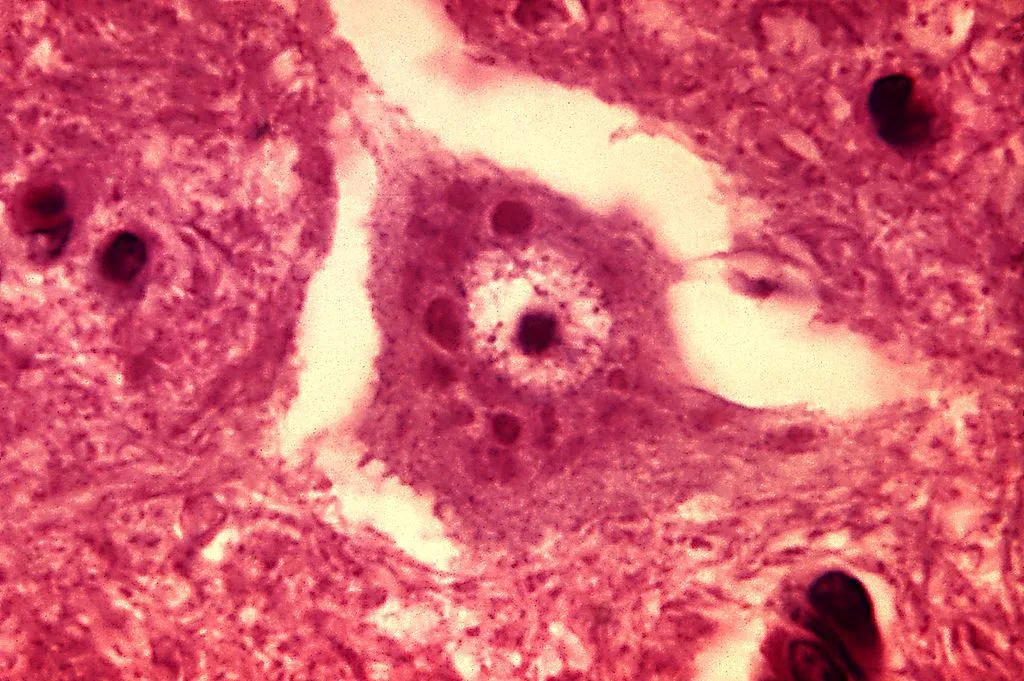
As the patient becomes hyperactive and hydrophobic, they also begin to salivate—a lot. The virus moves to the salivary glands and into the saliva in the next few days. The virus is ready to get transmitted to its next host.
The only problem for the virus is getting from the saliva into another host.
What Causes The Hydrophobia In Rabies?
What does salivation have to do with hydrophobia? Everything.
The rabies virus’s survival depends on jumping from one host to another. The best way to jump hosts is 1. get eaten, 2. get inhaled, or 3. enter through a wound or another orifice. The rabies virus uses option 3.
From the virus’ point of view, it is counter-intuitive to swallow. The virus-rich saliva cannot infect another host from inside the first host’s gut. Keeping the mouth flooded with saliva gives the virus the best offensive chances of being passed along.
Hydrophobia is less a fear of water and more a fear of the intense pain of swallowing water.
All of this leads to the introductory scene of the mad dog. The aggression and urge to bite something living is an ingenious form of viral manipulation.
The hydrophobia is brought on by the extreme pain of swallowing liquids, not just water. The virus causes intense muscle spasms in the throat that are excruciating, so much so that even the thought of swallowing can result in aggressive behavior.
Therefore, rabies does not create an irrational fear of water, as it is natural to be afraid of something you know will cause pain. Coupled with aggression and hyperactivity, anytime a rabies patient thinks or sees water, they startle and react violently, which might result in a bite.
Not all cases of rabies cause hydrophobia. There are two ways rabies manifests, depending on which strain of rabies virus one is infected with. The types are furious rabies and paralytic rabies. Furious rabies results in hydrophobia and aggression. Paralytic rabies, as the name suggests, results in paralysis of the limbs and, if not treated, can result in a coma.
Is There A Cure For The Rabies Virus?
Louis Pasteur found that infecting people with a weaker version of the virus (which he got from constantly reinfecting the virus in animals) could inoculate or vaccinate those people against rabies. Today, we have more sophisticated and quicker methods of treating rabies.
An individual bitten by a rabid or even suspected rabid dog then they’re put on a vaccination regimen. According to the CDC (Center for Disease Control and Prevention), “If you have not been vaccinated against rabies in the past, you need four doses of rabies vaccine over two weeks (given on days 0, 3, 7, and 14). You should also get another medication called rabies immunoglobulin on the day you receive the first dose of rabies vaccine or soon afterward.”
Rabies was thought to have a 100% mortality rate once the virus reached the brain. In 2011, a high school girl survived rabies without a vaccine. The doctor treating her developed a protocol to try to save her, and it worked! This protocol is now called the Milwaukee protocol and has reinvigorated curiosity in the treatment and strategy of this disease.
There is a lot we still don’t know about rabies. We know that the virus invades neurons and makes its way to the brain. We also know how the brain looks after an invasion, but the exact mechanism of how a virus goes about infecting the brain. We’re still investigating which parts of the brain the virus targets, and that leads to the disease’s unique symptoms.
Regardless, you can sleep soundly knowing that treatment is available.
References (click to expand)
- How rabies 'hijacks' neurons to attack brain.
- Rhabdoviridae - an overview | ScienceDirect Topics.
- Jackson, A. C. (2015, July 3). Mind-altering microbes. Journal of NeuroVirology. Springer Science and Business Media LLC.
- The Path of the Rabies Virus | Transmission.
- Pearce, J. (2002, July 1). Louis Pasteur and Rabies: a brief note. Journal of Neurology, Neurosurgery & Psychiatry. BMJ.
- Baer, G. M. (2017). The Natural History of Rabies. Routledge
- Is Rabies Really 100% Fatal? | Viruses101.
- Rabies Information | Mount Sinai - New York.
- Hemachudha, T., Laothamatas, J., & Rupprecht, C. E. (2002, June). Human rabies: a disease of complex neuropathogenetic mechanisms and diagnostic challenges. The Lancet Neurology. Elsevier BV.
- Rupprecht CE. Rhabdoviruses: Rabies Virus. In: Baron S, editor. Medical Microbiology. 4th edition. Galveston (TX): University of Texas Medical Branch at Galveston; 1996. Chapter 61. Available from: https://www.ncbi.nlm.nih.gov/books/NBK8618/
- Gluska, S., Zahavi, E. E., Chein, M., Gradus, T., Bauer, A., Finke, S., & Perlson, E. (2014, August 28). Rabies Virus Hijacks and Accelerates the p75NTR Retrograde Axonal Transport Machinery. (M. J. Schnell, Ed.), PLoS Pathogens. Public Library of Science (PLoS).