Table of Contents (click to expand)
A significant fraction of bacteria that actually inhabit our oral cavity are ‘friendly’ bacteria. Saliva plays a crucial role in ensuring that the nasty bacteria present in our mouth don’t make the wound any worse. That’s why wounds and cuts inside the mouth so rarely get infected by bacteria.
When you injure yourself or sustain a minor cut or bruise on your body, the wound usually heals itself in a week or two (depending on the nature and severity of the wound). In general, cuts and scrapes on most parts of the body take around the same amount of time to heal. To prevent the wound from getting infected, we clean it thoroughly, put some antibacterial cream on, slap a Band-Aid over it and call it a day
But what about injuries in the mouth?
When we bite our tongue accidentally, we rarely apply any antibacterial creams or even gargle with mouthwash. We simply brave the pain and move on.
This seems pretty remarkable, considering that our mouths are filled with millions upon billions of bacteria. There are more than 700 different strains of bacteria that can inhabit the human mouth, but most humans don’t host more than 35-70 varieties of these bacteria at any given time.
Many of these bacteria are just along for the ride. Our mouth is a fantastic place for microbes, as it’s warm, moist, and the food we eat has all the nutrients they could possibly need. Some microbes can be useful in limiting the growth of pathogenic bacteria. It’s important to note that this dynamic of ‘mutual help’ is maintained only when the host individual is healthy.
Many people expect an injury—a direct portal into the body—would be attacked by all the bacteria within our mouths and cause a severe infection, but that rarely happens. You’ll probably get a cavity before the bite on your cheek gets infected.
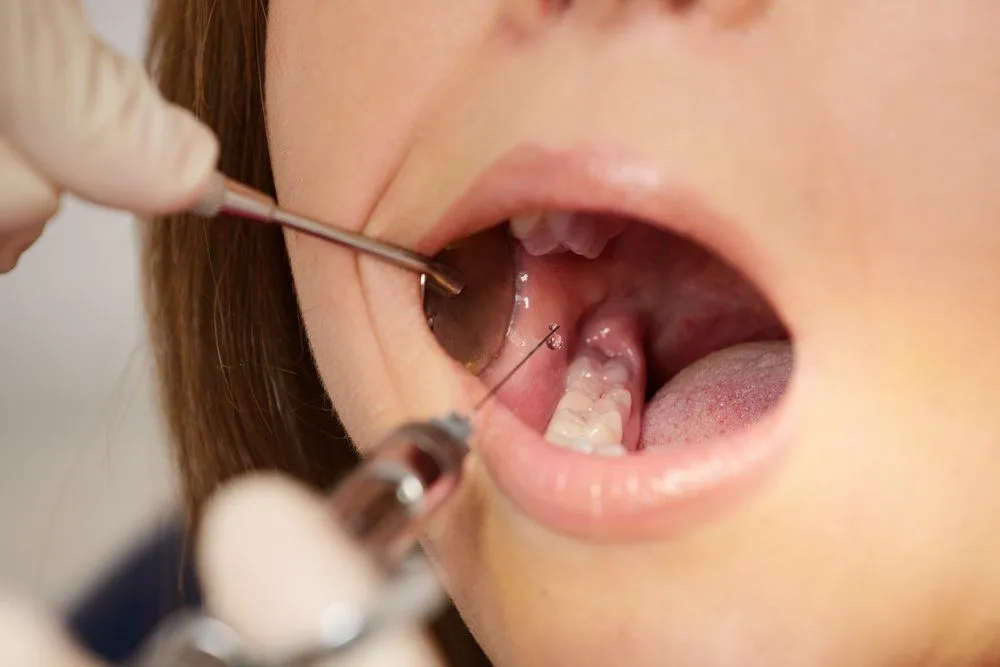
The interesting question is why? Why don’t the injuries within our mouths get infected?
Recommended Video for you:
Mouth-watering Solutions
The next time you bite your tongue or cheek, notice that there is often a rush of saliva into your mouth, almost immediately bathing the wound. Saliva isn’t just there to make food mushy enough to swallow; it has a host of different functions, many of which involve making sure your mouth doesn’t become a bacterial cesspool.
Saliva is rich with a host of different antimicrobial proteins, such as lysozymes, hydrogen peroxide and lactoferrin, just to name a few. These enzymes regulate the microbial load within the mouth, killing off potentially pathogenic and even normal oral microbiota.
Smaller than proteins, antimicrobial peptides are part of the bacteria-killing arsenal. Histatins, defensins and cathelicidins are all antimicrobial peptides with bacteria- and fungi-killing properties. The peptides have a positive charge, which allows them to attach to the negatively charged bacteria cell wall (or surface) and create pores that kill the microbes.
Besides these enzymes and peptides, certain other proteins can attach to multiple microbes. This prevents those microbes from attaching to a surface in the mouth and subsequently being swallowed.
How Wounds Heal
Keeping the mouth “clean” isn’t the only strategy to keep infections at bay. Oral wounds have been noted to heal faster than other wounds to the skin would, and with significantly less scarring. This fast “patch-up” job might prevent the wound from being exposed long enough for pathogens to begin their work.
The process for wound healing and tissue regeneration roughly follows the same steps, whether it be the skin on your arm or inside your mouth.
Immediately after a cut, ruptured blood vessels begin to seal up through coagulation at the wound site, which stops the bleeding. Injured skin cells secrete many different molecules that recruit immune cells to kill microbes and destroy any other foreign particles and begin inflammation of the tissue, which is important in healing a wound. A host of different cells begin to repair and regenerate the skin and the ruptured blood vessels. This is a slower process.
The skin in the oral cavity, though largely similar to skin elsewhere, has a few notable differences. First, the saliva in the mouth creates a thin film over the oral cavity, which lubricates the cells and prevents them from drying out. This lubrication is important for wound healing, giving cells the perfect environment in which to regenerate.
Our saliva also contains cytokines, chemicals that recruit immune cells and begin the process of inflammation and re-epithelialization (the process where new skin cell replace damaged cells). Histatins, along with their antimicrobial properties, have also been found to play a role in wound healing.
A paper published in 2018 in the journal Science Translational Medicine studied the differences in protein synthesis between oral keratinocytes and skin keratinocytes. They found that the transcription of certain proteins involved in wound healing were up-regulated in keratinocytes of the oral mucosa. This could be important, the researchers state in their paper, for understanding how to heal wounds faster and with minimal scarring.
Suffice to say that saliva plays a crucial role in ensuring that the nasty bacteria present in our mouths don’t make wounds any worse. That’s why wounds and cuts inside the mouth so rarely get infected by bacteria. However, this is only true for healthy individuals. More specifically, if a subject is suffering from some affliction to begin with, then the relation between the mouth bacteria and the body is severely affected. As a result, cuts and injuries within the mouth might not heal as swiftly as they usually do!
References (click to expand)
- Dawes, C., Pedersen, A. M. L., Villa, A., Ekström, J., Proctor, G. B., Vissink, A., … Wolff, A. (2015, June). The functions of human saliva: A review sponsored by the World Workshop on Oral Medicine VI. Archives of Oral Biology. Elsevier BV.
- Gorr, S.-U. (2009, October). Antimicrobial peptides of the oral cavity. Periodontology 2000. Wiley.
- Rodrigues Neves, C., Buskermolen, J., Roffel, S., Waaijman, T., Thon, M., Veerman, E., & Gibbs, S. (2019, May 2). Human saliva stimulates skin and oral wound healing in vitro. Journal of Tissue Engineering and Regenerative Medicine. Hindawi Limited.
- Morgan-Bathke, M., Martin, K., & Limesand, K. H. (2014). Salivary Glands and Saliva. Reference Module in Biomedical Sciences. Elsevier.
- Iglesias-Bartolome, R., Uchiyama, A., Molinolo, A. A., Abusleme, L., Brooks, S. R., Callejas-Valera, J. L., … Morasso, M. I. (2018, July 25). Transcriptional signature primes human oral mucosa for rapid wound healing. Science Translational Medicine. American Association for the Advancement of Science (AAAS).