Table of Contents (click to expand)
Epidurals are combinations of analgesics and pain relievers that can be applied during childbirth to mitigate the pain by blocking pain signal transmission in the spinal cord. While the use of epidurals and other drugs during childbirth is criticized by some on various grounds, and can have some minor side effects, they are an effective way to minimize the intense pain of the birthing process.
If you have personally given birth to a child, been in the room during a birth, heard about the experience from someone else, or simply watched the depiction of childbirth in movies or TV shows, you know that it is a uniquely beautiful and potentially excruciating act. The images of a mother’s face drenched in sweat, being told to “push” through the pain of labor, as she squeezes her partner’s hand into a pulp, are things that most of us have seen before.

However, modern medicine has progressed to the point where much of the pain of childbirth can be mitigated or blocked through various strategies, medications and minor procedures, including the use of an epidural. Before you decide whether to use an epidural during labor, or if you’re simply curious about this aspect of childbirth, the information below should clear up any uncertainty!
Recommended Video for you:
What Is An Epidural?
An epidural is a pain-relieving shot that many women receive during labor that effectively works as a nerve block. This nerve-blocking shot is called an epidural because it is injected into the epidural space, which is located directly outside the membrane encasing your delicate spinal cord. By numbing the spinal nerves, an epidural is also able to prevent pain signals from being transferred to the brain. This procedure is not solely used during pregnancy, but also in the case of various surgeries (spinal and otherwise), and for the management of chronic pain. Unlike a general anesthetic, an epidural will allow for muscle function, and for sensitivity to pressure and touch, even enabling women to stand and walk around, but will block the majority of pain.
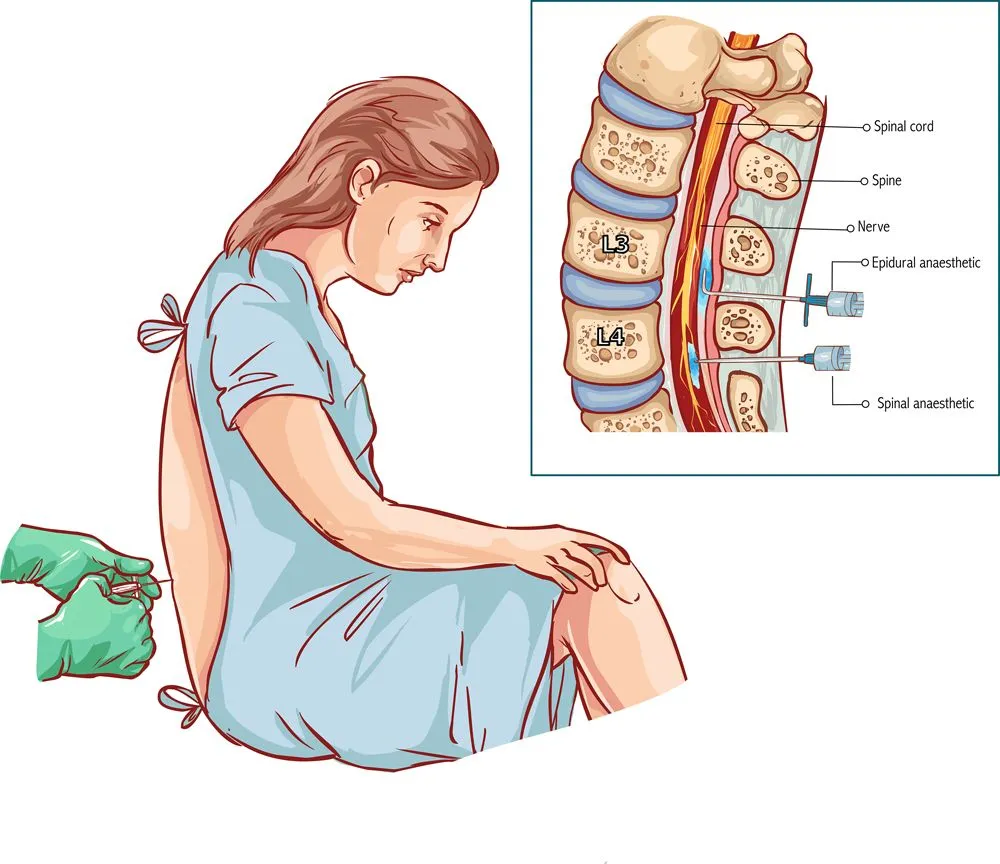
Epidurals come in a number of forms, including local epidurals, narcotic epidurals, local/narcotic mix, patient-controlled epidurals, continuous epidurals and intermittent epidurals. We will go into greater detail about these varieties below so the differences can be made clear.
Epidurals can be administered as a single injection, but this is often insufficient. For this reason, a catheter is usually attached to the injection site on the back, so additional medication can be easily delivered during the sometimes lengthy labor process.
Local Epidural
This is a standard or classic epidural, and consists of using normal local anesthetics to provide powerful pain relief. This form of epidural is often injected directly into the lumbar area of the back, into the fluid surrounding your spinal cord. This will provide numbness from the waist down, takes roughly 10-20 minutes to begin working, and can last for one to two hours. While this is an effective and trusted approach, it will reduce a woman’s ability to feel and push the baby out, and the initial stages of labor may take longer. This approach is also known as a spinal block. Some other side effects include the inability to walk during labor, lowered blood pressure and may increase your need for a Caesarean birth.
Narcotic Epidural
Also known as a “walking epidural”, this approach only uses pain-relieving medication, such as fentanyl or morphine, rather than providing any nerve blockage. The benefit of this approach is that it allows women to walk around and be mobile during labor, which can further help to relieve pain and stress, and may encourage a shorter labor. This can be an effective epidural, and may provide pain relief for 4-24 hours, depending on the chosen medication and the concentration. In some cases, babies are somewhat sedated upon birth, and may be sleepy for a few days, as well as less willing to feed, because their bodies are trying to process out the narcotic.
Local/Narcotic Mix
The most common epidural in use today is a mix of local anesthetics and narcotic medications, allowing for some muscle control and function from the nerves, but also providing adequate pain relief. The potential side effects of a “sedated” baby are minimized with this combination, and mothers are better able to push and even walk around. While side effects are still possible with a mixture, this is generally considered to be a well-balanced strategy.
Patient-Controlled, Continuous And Intermittent
In some cases, patient-controlled epidurals are called for, in which the release of narcotic medication through an IV into the catheter is determined by the patient. If you are experiencing a long labor, this might be an option. Also, there is a lock-out setting on the handheld release trigger to ensure that you don’t overmedicate yourself.
Intermittent epidurals can be “topped up” throughout the course of your labor if you have had a catheter injected and secured to your back. When the pain begins to return, the nurse or attending physician can easily administer more of the medication with a lag time of only a few minutes.
Continuous epidurals include the use of an IV bag and continuous, low-dose delivery of medication into the catheter. This is often preferred, because it reduces the swells of pain and relief that intermittent epidurals can cause.
Epidural Side Effects
There is a great deal of debate over the use of epidurals due to their potential side effects, some of which were explained above. While the idea of “sedating” your newborn baby or being unable to move during labor sound quite worrying, there are a number of other side effects to consider before deciding to use an epidural during labor.
The use of opioids in any context can result in certain side effects, such as topical itching of the skin and nausea or vomiting. The sedative nature of these drugs can also cause a drop in blood pressure, as well as fever or general soreness after the birth is over. Again, due to the numbness, some women have trouble urinating, or may become incontinent, as they are unable to tell when their bladder is full.
Some of the less common, but more serious side effects of using epidurals include nerve damage, infections, severe headaches, and respiratory issues. As mentioned above, the use of a local epidural can also extend the second stage of childbirth, once the cervix is fully dilated.
Epidural Controversy
The advancement in epidurals over recent decades is remarkable, and when used properly and responsibly, they are widely considered safe and effective pain-management tools. However, there are many other approaches to pain management and mitigation that doesn’t involve the use of narcotics or anesthetics. Human beings have been giving birth for tens of thousands of years without the help of such medicine, and many holistic practitioners and believers in natural medicine are staunchly against the use of drugs during childbirth.
While there are some risks to the use of an epidural, there is also something to be said for relieving pain when possible, particularly during a process often described as the most painful event a human can endure. Some people argue that deep breathing practices, support from a doula or birth partner, water immersion births, acupuncture, meditation and many other drug-free strategies will provide a more natural birth experience. There are positive and negative points on both sides, so ultimately, the decision to use or refuse an epidural is entirely personal. Be sure to discuss your decision with your doctor, along with your preferences and concerns, well before you go into labor!
A Final Word
Childbirth is a miraculous and momentous event in a woman’s life, but as the word “labor” implies, it takes a lot of work and perseverance through incredible pain. Epidurals, in various forms, can provide relief from the most severe discomfort of this magical moment, while also protecting the health and wellness of both mother and child.
References (click to expand)
- Birth: Learn More – Epidurals and other medications to ....
- Epidural – Everything You Should Know About It.
- Labor, S., & Maguire, S. (2008, December). The Pain of Labour. Reviews in Pain. SAGE Publications.
- Dozier, A. M., Howard, C. R., Brownell, E. A., Wissler, R. N., Glantz, J. C., Ternullo, S. R., … Lawrence, R. A. (2012, June 13). Labor Epidural Anesthesia, Obstetric Factors and Breastfeeding Cessation. Maternal and Child Health Journal. Springer Science and Business Media LLC.